by Marissa Mangual, LPCMemorial Day marks the unofficial beginning of summer. Typically we see lots of images about "summer body" which can stir up feelings of shame or inadequacy especially after all these weeks of being in quarantine. I think about how we each have a different relationship to food. Some of us eat enough to nourish ourselves. Some of us have shame around food that we learned from our families, friends, media. Some of us have strict rules around what we can eat and when we can eat. Some of us use food to comfort ourselves when we are feeling sad, bored, lonely, angry, anxious. Some of us think we will feel better when we reach a certain size or body shape and have learned extreme ways to try and achieve that. We each can have periods where we eat too much or too little. Stress, isolation, lack of control, not feeling worthy can lead to disordered eating. Eating disorders are ultimately not about food but about our relationship to our feelings, the people around us, and willingness to be flexible and not always in control. Living through a pandemic can make us more vulnerable.
Another impact from quarantine is the disruption of effective coping skills. Some people developed coping skills that mainly involved socialization and not isolating. Some skills and distractions may have been going to bookstores, hanging out with friends and family, enjoying nature or hiking, seeing a movie, or perhaps going to a coffee shop. These are common and helpful coping skills for many. Those in early recovery may also be working on exposure by going into restaurants and ordering new foods. It can be challenging to adapt and learn unfamiliar coping skills when the ones that worked are temporarily unavailable. In turn, this may increase uncertainty and feeling out of control. However, you can still do this! There are resources available online and tips to help. Many people with eating disorders also struggle with co-occurring disorders including substance use, depression, anxiety, trauma, and/or mood disorders. When someone attempts to manage ED behaviors they may have urges to use substances or engage in other harmful or ineffective behaviors as well. Trying to cope with various urges and uncomfortable emotions during social distancing could magnify symptoms of anxiety and depression. In turn, these symptoms could increase ED behaviors or lead to relapse. What is wonderful is most people’s access to technology and the various platforms for video chats. There are ways to stay connected and receive support and therapy through Telehealth (online) services. Thankfully, even insurance companies are making accommodations for providers and members to make it more accessible and easier at this time. Additionally, multiple support groups have become available online if you do not have a support network around you. I have noticed an insurmountable amount of posts on instagram and social media about weight gain during quarantine. I feel that some people speak of this anxiety as if it is equal to the fear of infection itself. There has been an incredible amount of commentary and messages about “eating healthy” and “being more productive” to stay fit during this time. It is okay to have feelings about weight gain, feelings are always valid, but society as a whole puts incredible pressure and indirect shame for being stationary and putting on pounds for enjoying foods and eating more than one may typically eat. Most of these messages are under the veil of a joke. Shame and guilt can be driving forces to an eating disorder. For me, I have to limit and block some accounts to avoid seeing and internalizing these messages. I also spread awareness and follow accounts from ED dietitians, therapists, and other like-minded individuals. I suggest taking time away from social media or diet-culture accounts if you find it it influences you more negatively during this time. As we continue to social distance and stay safe, I want to also remind everyone that it is OKAY not be okay right now. The world is experiencing a collective trauma that no one could have psychologically and emotionally prepared for. With that said, it does not mean you lack complete control. You may cope differently, experience more sadness and anxiety than usual, and struggle to stick to a regular meal plan. However, human beings are innately resilient and capable of adapting to even the most unpredictable circumstances. Reach out for support Be kind to yourself. You can get through this. We are here for you and your family. Learn more about how to contact us here and read more about eating disorders.
1 Comment
by Marissa Mangual, LPC The Coronavirus (Covid-19) has impacted the world financially, socially, economically, medically, and psychologically. My first concern has been the lives of those impacted by this virus, but I also began thinking about the influence on individuals struggling with eating disorders and recovery.
There are several reasons why people with eating disorders are more vulnerable and at risk for relapse during this pandemic. The coronavirus has created fear and heightened anxiety in the general population. It has increased feelings of instability and being out of control. Many with eating disorders have a desperate need to control aspects of their lives including their environment and unpleasant emotions. This control takes form through engaging in behaviors such as restricting food, binge eating, purging, over-exercising, and taking diet pills/laxatives. The necessary precautions that our nation has put in place may cause a significant increase in feeling out of control in multiple areas. These areas may include dealing with a loss in job/change in job structure or location, financial burdens, lack of resources or supplies, closings of recreational activities and groups, and lack of connection and socializing. As a result, this can increase isolation, symptoms of depression and anxiety, lack of self care, decline in managing daily responsibilities, changes in sleep and eating patterns, and increase in eating disorder behaviors. How may these changes affect your eating disorder recovery? Being quarantined leads to isolation and lack of connection. This can increase feelings of sadness, hopelessness, anxiety, irritability, restlessness, and an array of other emotions. Additionally, the restrictions in movement and exercise may perpetuate the fear of gaining weight, maximize the amount of body checking, and ultimately lead to urges or engagement in restricting food in an effort to control weight gain. Additionally, many people are stocking up on food due to supplies quickly running out at stores as well as limiting time spent at markets. With this said, kitchen cabinets are filled more with foods that could trigger binge eating behavior. Those in recovery may have specific meal plans but may have to change where they shop and what foods they purchase. As someone in recovery from an eating disorder, we are taught how to stray from ‘safe foods’ and learn there is no”good” or “bad”. With that said, I have experienced complete terror when attempting to buy 2% milk instead of 30 calorie almond milk. I have a vivid memory of standing in the dairy aisle for 10 minutes just trying to gain the courage to fight my ED mind and buy what my body needed for nutrition. So, I get it my fellow ED warriors. For someone in early recovery, the sudden change may feel catastrophic. It may lead to avoiding buying food all together and/or restricting. However, there are plenty of options and alternatives that will meet a given meal plan, I promise you (this does not include medical reasons for food choices). Remind yourself that not every meal is going to be perfectly balanced. Personally, a big trigger of mine is isolation and boredom. I had a tendency to overeat to compensate for loneliness and lack of stimulation. I would temporarily feel better, of course, but guilt and shame inevitably followed. Because of the guilt from bingeing, I would often compensate by restricting the following day in an attempt to alleviate those feelings. Again, I would temporarily feel better but risked bingeing at night which led to further guilt. Ultimately, this perpetuated the cycle. The social distancing, gym closures, and increase in mental health issues also make it difficult to break the cycle. Also, sudden job losses and financial burdens can hinder individuals from receiving therapy or taking a hiatus until it becomes more affordable. There are many free webinars, talks, groups, and services that are popping up all over the internet. Check out some links at the bottom of this site as well our page on eating disorders. Reach out to us for a consultation and support. Call or email. You can read more about Marissa Mangual here who specializes in treatment of disordered eating. Resources: Coping in Isolation with an Eating Disorder Online Support Groups 5/3/2020 5 Comments Stages of Griefby Emily Suzuki, MA, LAC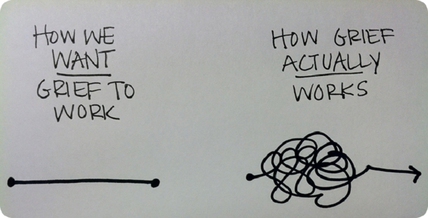 How are we as individuals and as a collective experiencing grief? Covid-19 has brought us into unchartered territory. Even as many of us shelter in place, and limit our mobility we feel as though we are navigating ways and places that we have never before had to face. Overwhelming feelings are common right now and need our attention and compassion more than ever. Everyone is struggling with a loss of normalcy. Our daily routines are turned upside, family, friends and co-workers are missed and each of us is being asked to restructure the ways we spend our time and how we move through the world. Many are mourning loved ones passing. Our sense of safety has been pushed to the edge, and ultimately, we are becoming more intimate with our fears of death and dying. As we work through this time, it makes sense that we are experiencing the stages of grief. Elizabeth Kubler Ross and David Kessler outline the stages in their book On Grief and Grieving: Finding the Meaning of Grief through the Five Stages of Loss. The stages include denial, anger, bargaining, depression and acceptance. The process of grief evolves in its own time and way depending on each individual and circumstance. There’s no clear roadmap. Often, it’s not linear, it can take much longer than we want it to, and it can feel quite messy. Denial is the first stage. According to Kübler-Ross and Kessler “denial helps us survive the loss.” It gets us through the initial days and weeks of shock and acts as a kind of filter, only allowing us to acknowledge what we’re ready to handle. As much as denial is the act of looking in the opposite direction, there is a wisdom to it too. In an already overwhelmed state, denial allows us to turn towards our grief when we’re ready. Feeling anger is a sign that there are many other emotions percolating under the surface of grief. In the state of overwhelm and feeling lost, anger is recognizable, and something we can hold onto easily. In fact, too often it’s what sticks and sticks around for a long time. Here, we look externally, for ways to point the finger at someone or something to blame. It’s familiar and easier, than managing the deeper emotions of grief. Anger is also a protector and can point to the things we value and care about and ultimately, what we love and don’t want to lose. Kübler-Ross and Kessler explain the stage of bargaining as the attempt at a “temporary truce.” In this stage we ask ourselves a lot of “what ifs” and wonder “if only”. We try to negotiate with the pain we’re feeling and can feel a sense of desperation and longing for returning to a way before change and loss. An attachment to our previous sense of normalcy, and in this stage, we really resist the reality of the beginning of a new normal. Depression arrives when “our attention moves squarely into the present.” This stage is difficult, and feelings of emptiness and hopelessness can arise. It can feel endless, and without light at the end of the tunnel, we feel truly lost at sea. Like every stage, depression takes the time it takes for any given individual. In our society, there is stigma around extended grief. We are expected to wrap up and move on within a certain, very short, period of time, and get back to the day to day. Bereavement is a normal and healthy part of grieving and it is important not to confuse or label it as mental illness. Finally, in our own time, we experience the stage of acceptance. Here, we begin to acknowledge that there is no going back to before, and we tentatively learn to adjust and reorganize ourselves around this new reality. This doesn’t happen overnight, and maybe only takes the shape of momentary ease but eventually acceptance builds and accumulates into longer stretches of time. Feelings of guilt can come up as we recognize ourselves moving forward, but we begin to trust that we can both honor the absence of what we have lost, while also allowing ourselves to grow and change. Recognizing that we are ALL in some way experiencing grief and loss during this unusual time, we must turn our attention inward. Looking inside, we can ask ourselves, what am I feeling right now? What have I lost and what am I afraid of losing? This leads us to reflect on what do I love and value? What do I hold most dear and how can I honor them if and when I have to say goodbye? These questions are difficult and uncomfortable, and often quite painful. Grief is a heavy weight to carry, and you do not have to carry it alone. For support and to see how we can support you during this time of loss and transition please call us or read more about our team at Mindful and Multicultural Counseling. 4/20/2020 3 Comments Befriending limiting beliefsby Nathalie Edmond, PsyD, E-RYT What does it mean to move from surviving to thriving? I ask myself a variation of this question regularly. How do I even know when I am just surviving. I think about surviving as living from a fear or shame-based place. My stress response is firing and saying we have to do certain things to just get our basic needs met. There is some sort of external threat that we have to navigate. Living through a pandemic will automatically trigger our desire to survive, by any means necessary. I have found that crises, like pandemics, tend to exaggerate patterns, behaviors, feelings that are already there. If we tend to be pretty laid back, like myself, that may be exaggerated and I may not take pandemic precautions as seriously. If I tend to be more anxious and not like uncertainty I may be more anxious now and may find other ways to try and control my environment in order to calm my nervous system.
A little bit of fear is good. The fear propels us into action. Perhaps that gets us to stay at home, wear a mask in public places, take extra precautions to take care of ourselves, our families and our community. Too much fear moves us into scarcity mindset and parts of our brain go to sleep and are not available to us. Our frontal lobes tend to go to sleep when we operate in extremes of emotion (too much or too little) Our frontal lobes are responsible for long term planning, compassion, awareness, impulse control, maintaining dual awareness and soothing our fearful parts. I have been doing some personal exploration in recent months in order to see where I let fear take over my life, particularly in my work life. David Bayer, a business coach, talks about how we can shift to a more powerful state of being and living where are limiting beliefs don’t drive our decision making. Limiting beliefs are stories we tell ourselves that get in the way of us reaching our potential or imagining what we think is possible in our lives. Here are some examples of limiting beliefs:
Joseph Sanok, another business coach, suggests living from a place of experimenting rather than pass/fail. That means we allow ourselves to see life as an experiment and not be so attached to the outcome. Through my meditation practice I have learned that my attachment to the outcome is usually what causes me to suffer. If I focus on actions I am taking and am trusting of the universe I can shift into an abundance mindset rather than a scarcity mindset. My scarcity mindset says it won’t work out if I don’t hold on to old ways of being. If we experiment, we may try a new behavior such as taking a certain risk and see how it goes. We take the information we get from the experiment and decide if we want to continue with it or if we want to make an adjustment. An example I have from a couple of years ago where I tried this experiment- I wanted to reduce the number of evenings I worked so I could spend more time with my family. I changed my outgoing voicemail to reflect that I was only taking new clients in the daytime. I was worried that placing that kind of limit on my work schedule would lead to me not getting new clients and hence make less money. I decided to challenge myself and try it out for a couple of months and ride the wave of anxiety and limiting thoughts. I was able to fill my daytime hours and phase out most of my evenings. Last summer I took the risk of expanding from my solo practice to a group practice. I had so much fear I started chanting every day to help redirect my energy and thoughts so I can approach the fear rather than running from it or playing it too safe. There are many ways to break free from our limiting beliefs and help our frontal lobes be online more of the day- therapy, yoga, meditation are just some of the paths we can help you with. If you want help identifying and working through your limiting beliefs or navigating your emotions related to COVID-19 our team at Mindful and Multicultural Counseling is here to help. Call us or read more about us here. 3/6/2020 14 Comments Eating Disorder Awarenessby Marissa Mangual, LPCFebruary 24 through March 1 marks Eating Disorder Awareness Week. According to the Association of Anorexia Nervosa and Associated Disorders (ANAD) and National Eating Disorder Association (NEDA), eating disorders affect about 30 million people of all ages, races, ethnicities, and genders in the US. It is considered to have the highest mortality rate of any mental illness, with at least one person dying every 62 minutes from an eating disorder. On average, about 50% of those diagnosed with Anorexia Nervosa, Bulimia Nervosa, and Binge Eating Disorder have co-morbid mood disorders, anxiety disorders, and/or substance use disorders. It is also not uncommon for one who has experienced trauma/PTSD to develop an eating disorder as well. Even for someone who has personally struggled with eating disorders for about 12 years now, in addition to treating many clients who have struggled with such disorders as well, the statistics remain shocking to me. Eating disorders have an incredible impact on an individual’s physical, mental, and emotional well-being.
Eating disorders are incredibly complex: and researches are still studying the causes and developments of such disorders. Body image, weight, shape, and relationships with food are all common factors, however, they are also attempts to cope with, and gain control over, overpowering and painful emotions. But like any other mental health disorder, no one person is the same despite experiencing similar symptoms. Identifying what emotions and triggers drive the behaviors are key, in addition to developing helpful tools to learn to manage the emotions, thoughts, and behaviors that perpetuate the cycle. This is an ongoing process that is not easy by any means, but it IS possible. The hardest piece about it is that we have to eat every day in order to fuel our bodies with the nutrients that it needs. It may feel like an impossible and scary feat, but we are more capable of recovery than we give ourselves credit. For someone who has struggled with eating disorders since college, asking for help was the scariest, and best, thing I ever did for myself. Honestly, I was unaware that I had a problem all of those years. In my personal and professional experience, I notice how significant cognitive distortions can alter the way one views eating patterns, behaviors, and body image. One may start to feel incredibly guilty about what they eat, when they eat, how many calories they are consuming, and what they are putting into their body. A distinguishing feature of an eating disorder is the obsession and preoccupation with food throughout the day: followed by extreme guilt, shame, anxiety, anger, and sadness. These thoughts intensify the more malnourished our bodies become. In addition, having an eating disorder can be easy to hide, and the behaviors can be rather secretive. A common misconception is that someone with an eating disorder has a ‘frail, sickly’ body, or an ‘overweight, heavy body’. Remember, eating disorders can affect ALL bodies and sizes. Being on one side of the scale, or the other, also does not mean someone has an eating disorder. There can be numerous factors that impact size and weight. So, going back to asking for help, I often ask my clients, “What is the threat? What are your fears? What gets in the way of seeking help for ourselves?” Exploring the barriers that get in the way are incredibly important, and not just for one struggling with an eating disorder. Some things that get in the way are the stigmas associated with mental health, as well as feelings of shame, weakness, and fear of the unknown. It is a vulnerable experience to put yourself in the hands of a treatment team and allow yourself to travel down an unfamiliar path. I believe this is the most courageous act one can do for themselves. Taking a step to heal yourself and ask for help is brave and empowering. This does not mean you are not brave or capable if you are not ready. Perhaps I can suggest keeping an open mind to the idea of healing, and the possibility of receiving help. You are not alone. Schedule a consultation with me at Mindful and Multicultural Counseling to learn more about ways to heal. Resources: https://www.nationaleatingdisorders.org https://www.nationaleatingdisorders.org/screening-tool https://www.nationaleatingdisorders.org/help-support/contact-helpline https://anad.org https://www.eatingdisorderhope.com 2/15/2020 0 Comments Mindful sleeping habitsby Lina Lewis-Arevalo, LPC, LCADC Are you lying awake at night, tossing and turning, your mind swirling with distressing thoughts? Do you go to sleep at night, only to wake up at 3 am, unable to fall back to sleep? Did your doctor prescribe an anti-anxiety medication like a Benzodiazepine, or a sleep medication, either prescription or OTC, and you find it becoming less effective and needing to take more? Do you dread going to bed at night, expecting another restless night? You may be suffering from chronic insomnia.
|
Mindful and Multicultural Counseling Clinical TeamTherapists and psychologists committed to improving well being and mindful living. Archives
August 2023
CategoriesAll Addiction Anxiety Back To School Coronavirus Depression Eating Disorder Fear Meditation Mental Health Mindfulness Radical Acceptance Tapping Teenagers Therapy Transitions Yoga |
Mindful and Multicultural Counseling (609) 403-6359
20 Scotch Road, Suite E Ewing, NJ 08628








 RSS Feed
RSS Feed